Understanding COPD Symptoms: Key Signs and Causes
Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung condition that makes breathing difficult. It encompasses conditions like emphysema and chronic bronchitis. Recognizing the early signs and understanding the underlying causes of COPD is crucial for timely diagnosis and management, potentially improving quality of life for those affected. This article explores the common indicators and contributing factors of this widespread respiratory illness.
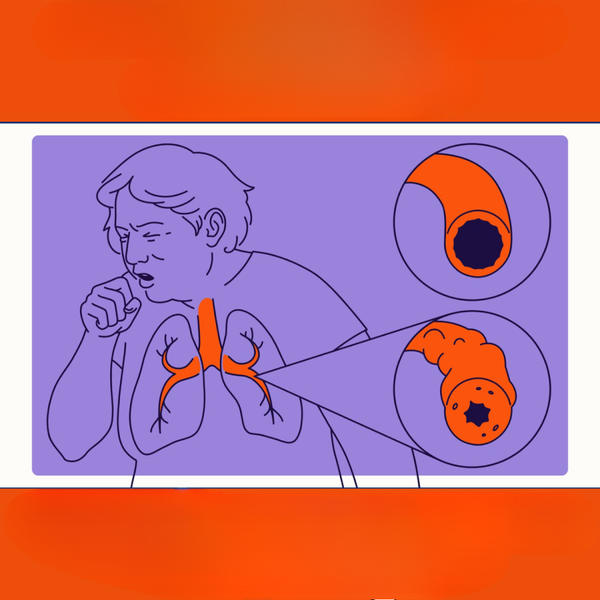
Recognizing Common COPD Symptoms
COPD often develops gradually, with symptoms worsening over time. Initially, individuals might dismiss signs as part of aging or a temporary ailment, especially if they are smokers. However, persistent symptoms warrant medical attention to ensure an accurate diagnosis and appropriate care plan. The primary impact of COPD is on the airways, leading to airflow obstruction and impaired gas exchange in the lungs.
One of the most characteristic COPD symptoms is shortness of breath, or dyspnea. This symptom may first appear during physical activity, such as climbing stairs or exercising, and gradually become noticeable even during routine daily tasks. As the condition progresses, individuals may experience breathlessness at rest, significantly impacting their mobility and independence.
A chronic cough is another prevalent indicator among COPD signs. This cough is often described as a “smoker’s cough” and may produce clear, white, yellow, or greenish sputum. The cough can be persistent throughout the day, sometimes worsening in the morning or during periods of respiratory infection. Increased mucus production in the airways contributes to this cough, as the body attempts to clear obstructions.
Wheezing, a high-pitched whistling sound during breathing, is also a common symptom, particularly when exhaling. This sound results from narrowed airways. Alongside wheezing, individuals may experience a feeling of tightness in the chest, which can further exacerbate feelings of breathlessness and discomfort. These respiratory signs collectively point towards potential lung function compromise.
Understanding the Causes of COPD
While the exact progression of COPD can vary, certain risk factors are strongly linked to its development. Understanding these causes is vital for prevention and for identifying individuals who may be at higher risk. The primary cause of COPD worldwide is exposure to airborne irritants that damage the lungs and airways over time.
Cigarette smoking is by far the leading cause of COPD, accounting for a significant majority of cases. Both active smoking and prolonged exposure to secondhand smoke can severely damage the delicate tissues of the lungs, leading to inflammation and destruction of air sacs (emphysema) and irritation of the bronchial tubes (chronic bronchitis). The longer and more heavily a person smokes, the greater their risk of developing COPD.
Occupational exposure to certain dusts, chemicals, and fumes can also contribute to the development of COPD. Workers in industries such as mining, construction, textile manufacturing, and agriculture may be exposed to irritants like coal dust, silica, cadmium dust, and chemical fumes. Adequate protective measures in the workplace are crucial to minimize these risks.
Air pollution, both outdoor and indoor, plays a role in the onset and exacerbation of COPD. Exposure to high levels of particulate matter from vehicle exhaust, industrial emissions, and burning biomass fuels (like wood or dung for cooking and heating in poorly ventilated areas) can irritate the lungs and contribute to chronic inflammation and damage over time. Indoor air quality, particularly in developing countries, can be a significant factor.
Genetic factors can also predispose individuals to COPD. The most well-known genetic risk factor is Alpha-1 antitrypsin (AAT) deficiency. AAT is a protein produced in the liver that protects the lungs from inflammation caused by infections and inhaled irritants. A deficiency in AAT can lead to early-onset emphysema, even in non-smokers, making this a critical consideration in the overall understanding of COPD symptoms and causes.
COPD Symptoms in Older Adults
COPD symptoms for seniors can often be more challenging to identify, as some of the early signs may be mistakenly attributed to normal aging. Reduced exercise tolerance, fatigue, and occasional breathlessness might be dismissed as typical age-related changes rather than indicators of an underlying lung condition. This can lead to delays in diagnosis and treatment, which are critical for managing the disease effectively.
Older adults with COPD may experience a more pronounced impact on their daily activities. Simple tasks like walking across a room, getting dressed, or preparing meals can become exhausting due to increased shortness of breath. This can lead to a significant reduction in physical activity, further contributing to deconditioning and a decline in overall health. Fatigue is also a common complaint, often linked to the increased effort required for breathing.
It is important for older adults and their caregivers to be vigilant about persistent respiratory changes. A chronic cough that lingers for weeks, recurring respiratory infections, or new onset of wheezing should prompt a visit to a healthcare professional. Differentiating COPD from other age-related conditions, such as heart failure or asthma, requires thorough medical evaluation, including lung function tests like spirometry. Early recognition of COPD signs in seniors can pave the way for interventions that improve breathing and maintain independence.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Recognizing the key signs of COPD and understanding its various causes are fundamental steps toward managing this chronic respiratory condition. While smoking remains the most significant risk factor, environmental exposures and genetic predispositions also play crucial roles. Early detection and intervention, especially for older adults where symptoms might be overlooked, can significantly impact disease progression and enhance an individual’s quality of life. Consulting with healthcare providers for persistent symptoms is always recommended to ensure proper diagnosis and care.




